Excretion Notes
O1. KIDNEY FORM AND FUNCTION
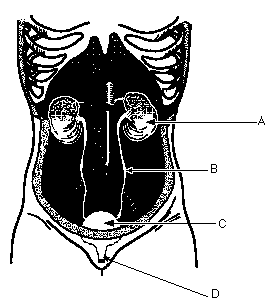
A. Kidneys:
- Produce urine
B. Ureters:
- Transport urine from kidneys to bladder
C. Bladder:
- Storage of urine
D. Urethra:
- Elimination of urine from bladder
Renal Cortex (outer layer of kidney)
- Contains glomerulus, proximal and distal tubules
- Pressure filtration, selective reabsorption and tubular excretion
- Responsible for most of the work of the kidney
Renal Medulla (inner layer of kidney)
- Contains loop of Henle, and most of the collecting duct.
- Responsible for H2O reabsorption and salt balance
O2. NEPHRON STRUCTURE AND FUNCTION
- Produce urine
B. Ureters:
- Transport urine from kidneys to bladder
C. Bladder:
- Storage of urine
D. Urethra:
- Elimination of urine from bladder
Renal Cortex (outer layer of kidney)
- Contains glomerulus, proximal and distal tubules
- Pressure filtration, selective reabsorption and tubular excretion
- Responsible for most of the work of the kidney
Renal Medulla (inner layer of kidney)
- Contains loop of Henle, and most of the collecting duct.
- Responsible for H2O reabsorption and salt balance
O2. NEPHRON STRUCTURE AND FUNCTION
Key and Functions
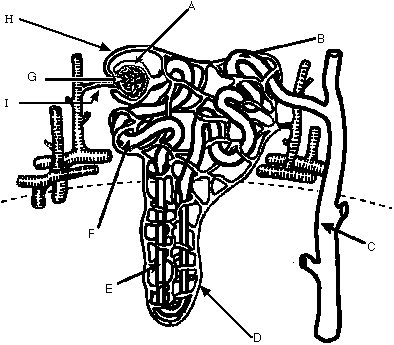
The kidney is composed of millions of tine separate tubules called Nephrons
G - Glomerulus capillary network in which a large portion of the blood plasma filters from the blood vessels into the Bowman's capsule
A - Bowman's Capsule collecting area for blood plasma from (filtrate) glomerulus. Blood is pressure filtered . (proteins, cells, large stuff stays in, salts sugar, waste etc. filter out)
I - Afferent arteriole blood vessel entering the glomerulus. Normal O2 blood.
H - Efferent arteriole blood vessel leaving the glomerulus. Goes to the capillary network. Thick blood, (less plasma etc)
D - Capillary network network of capillaries around the rest of the tubules. Reabsorbs nutrients, H2O etc.
F - Proximal Convoluted tubule - sugar and salts are actively transported out of filtrate (tubule) back into the blood (Capillary network) Uses ATP, O2. Walls are covered with microvilli.
- The filtrate is now less concentrated than the blood, so water moves from the filtrate to the blood by diffusion
E- Loop of Henle - dips down into medulla
- more H2O is absorbed into blood from decending limb
- Na+ and Cl- also reabsorbed
-Counter current exchange - salt (Na+ Cl-) is diffused and pumped out of the ascending limb and diffuses back into the decending limb. Also, urea diffuses out of the collecting duct and into the ascending limb. This adds to the hypertonic solution of the medulla and allows the kidney to excrete very hypertonic urine (concentrated)
B -Distal Convoluted Tubule
- some tubular excretion into tubule from blood
- a few materials are actively excreted from blood into tubules. (penicillin, histamines, H+, etc.)
C - Collecting duct - Common duct which collects filtrate from many distal tubules (Nephron)
- Very important in regulating the overall water content of urine
- Can control from very dilute urine (lots of water) to very concentrated urine, (very little water, most reabsorbed)
O3. BLOOD IN RENAL ARTERY AND VEIN
Substance Renal Artery Renal Vein
- Glucose - 100 mg/l - 98 mg/l
- Urea - 30 mg/l - 25 mg/l
Glucose is 100% reabsorbed from the filtrate into the blood. The 2 mg/l drop above is a result of sugar used to make ATP to fuel all the active transport that is happening in the tubules.
Urea is lower in the renal vein because it is excreted in the filtrate. Some is reabsorbed by the tubules. The kidneys do not remove all the wastes from the blood, they remove enough to keep the blood at a constant level. One kidney can actually be sufficient, a human can easily survive with only one. Sometimes people will donate a kidney to a close relative.
O4. ADH AND ALDOSTERONE
i) ADH - Anti Diuretic Hormone
- controls H2O balance
- ADH is secreted by the posterior pituitary gland
- increases the permeability of the distal tubule and collecting duct so that more water can be reabsorbed back into the blood.
- if ADH is secreted:
blood volume increases
blood becomes more dilute
urine becomes more concentrated
- ADH secretion is controlled by the water content of the blood. As blood conc. increases, more ADH is secreted, so more water is reabsorbed, and blood conc. then decreases.
ii) Aldosterone
- hormone secreted by adrenal cortex gland (outer layer of the adrenal gland on top of each of the kidneys).
- controls the excretion of Na+ and K+
- increases reabsorption of Na+ (inc. Na+ in blood)
- increases excretion of K+ (decr. K+ in blood)
- If blood Na+ level is too low, Aldosterone is secreted, reabsorption of Na+ by the kidneys occurs, so blood Na+ begins to increase.
- also controls blood volume (& pressure). Increase in Na+ in blood causes H20 to be reabsorbed, increasing blood volume & pressure
Role of Hypothalamus - area of the brain directly above the pituitary gland
The hypothalamus actually secretes the ADH which is released by the Posterior pituitary gland. The hormone is transferred and stored in a series of nerve cells which run from the hypothalamus to the post. pit. gland. The actual conc. (water) of the blood is monitored by the hypothalamus. If the blood is too concentrated, the hypothalamus triggers the post. pit. gland to release the ADH. The ADH increases the permeability of the distal tubule and collecting duct, so that more water is reabsorbed from the urine back into the blood. As the blood becomes more dilute, less hormone is secreted.
If the blood is too dilute, no ADH is released, the kidney tubules stay impermeable, so little water is reabsorbed (dilute urine) and the blood begins to become more concentrated.
Summary
- blood is too concentrated
- Hypothalamus triggers Posterior Pituitary Gland to secrete ADH
- more H2O is reabsorbed by collecting duct and distal tubule
- blood becomes more dilute
- blood is too dilute
- Hypothalamus causes less ADH to be secreted
- Little H2O is reabsorbed by collecting duct and distal tubule
- Blood becomes more concentrated
The kidney is composed of millions of tine separate tubules called Nephrons
G - Glomerulus capillary network in which a large portion of the blood plasma filters from the blood vessels into the Bowman's capsule
A - Bowman's Capsule collecting area for blood plasma from (filtrate) glomerulus. Blood is pressure filtered . (proteins, cells, large stuff stays in, salts sugar, waste etc. filter out)
I - Afferent arteriole blood vessel entering the glomerulus. Normal O2 blood.
H - Efferent arteriole blood vessel leaving the glomerulus. Goes to the capillary network. Thick blood, (less plasma etc)
D - Capillary network network of capillaries around the rest of the tubules. Reabsorbs nutrients, H2O etc.
F - Proximal Convoluted tubule - sugar and salts are actively transported out of filtrate (tubule) back into the blood (Capillary network) Uses ATP, O2. Walls are covered with microvilli.
- The filtrate is now less concentrated than the blood, so water moves from the filtrate to the blood by diffusion
E- Loop of Henle - dips down into medulla
- more H2O is absorbed into blood from decending limb
- Na+ and Cl- also reabsorbed
-Counter current exchange - salt (Na+ Cl-) is diffused and pumped out of the ascending limb and diffuses back into the decending limb. Also, urea diffuses out of the collecting duct and into the ascending limb. This adds to the hypertonic solution of the medulla and allows the kidney to excrete very hypertonic urine (concentrated)
B -Distal Convoluted Tubule
- some tubular excretion into tubule from blood
- a few materials are actively excreted from blood into tubules. (penicillin, histamines, H+, etc.)
C - Collecting duct - Common duct which collects filtrate from many distal tubules (Nephron)
- Very important in regulating the overall water content of urine
- Can control from very dilute urine (lots of water) to very concentrated urine, (very little water, most reabsorbed)
O3. BLOOD IN RENAL ARTERY AND VEIN
Substance Renal Artery Renal Vein
- Glucose - 100 mg/l - 98 mg/l
- Urea - 30 mg/l - 25 mg/l
Glucose is 100% reabsorbed from the filtrate into the blood. The 2 mg/l drop above is a result of sugar used to make ATP to fuel all the active transport that is happening in the tubules.
Urea is lower in the renal vein because it is excreted in the filtrate. Some is reabsorbed by the tubules. The kidneys do not remove all the wastes from the blood, they remove enough to keep the blood at a constant level. One kidney can actually be sufficient, a human can easily survive with only one. Sometimes people will donate a kidney to a close relative.
O4. ADH AND ALDOSTERONE
i) ADH - Anti Diuretic Hormone
- controls H2O balance
- ADH is secreted by the posterior pituitary gland
- increases the permeability of the distal tubule and collecting duct so that more water can be reabsorbed back into the blood.
- if ADH is secreted:
blood volume increases
blood becomes more dilute
urine becomes more concentrated
- ADH secretion is controlled by the water content of the blood. As blood conc. increases, more ADH is secreted, so more water is reabsorbed, and blood conc. then decreases.
ii) Aldosterone
- hormone secreted by adrenal cortex gland (outer layer of the adrenal gland on top of each of the kidneys).
- controls the excretion of Na+ and K+
- increases reabsorption of Na+ (inc. Na+ in blood)
- increases excretion of K+ (decr. K+ in blood)
- If blood Na+ level is too low, Aldosterone is secreted, reabsorption of Na+ by the kidneys occurs, so blood Na+ begins to increase.
- also controls blood volume (& pressure). Increase in Na+ in blood causes H20 to be reabsorbed, increasing blood volume & pressure
Role of Hypothalamus - area of the brain directly above the pituitary gland
The hypothalamus actually secretes the ADH which is released by the Posterior pituitary gland. The hormone is transferred and stored in a series of nerve cells which run from the hypothalamus to the post. pit. gland. The actual conc. (water) of the blood is monitored by the hypothalamus. If the blood is too concentrated, the hypothalamus triggers the post. pit. gland to release the ADH. The ADH increases the permeability of the distal tubule and collecting duct, so that more water is reabsorbed from the urine back into the blood. As the blood becomes more dilute, less hormone is secreted.
If the blood is too dilute, no ADH is released, the kidney tubules stay impermeable, so little water is reabsorbed (dilute urine) and the blood begins to become more concentrated.
Summary
- blood is too concentrated
- Hypothalamus triggers Posterior Pituitary Gland to secrete ADH
- more H2O is reabsorbed by collecting duct and distal tubule
- blood becomes more dilute
- blood is too dilute
- Hypothalamus causes less ADH to be secreted
- Little H2O is reabsorbed by collecting duct and distal tubule
- Blood becomes more concentrated