Reproduction Notes
REPRODUCTION
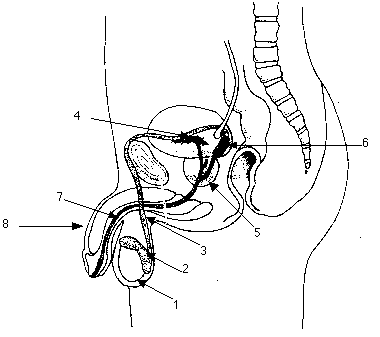
P1. Sructure and Function of the Male
P1. Sructure and Function of the Male
1) Testes
- outside abdominal cavity in scrotum
- sperm production needs < body temp
- sperm is produced inside tubes called seminiferous tubules
- interstilial cells also in testes produce male sex hormones -testosterone, and androgens
- maturing sperm are moved to the epididymis
2) Epididymis
- area where sperm mature (coiled tubes)
- then moved to the ductus (vas) deferens
3) Ductus (vas) deferens
- sperm stored here
- leads to urethra
- long tube from epid. to urethra
4) Seminal vesicles
- 2 small glands
- joins vas deferens at the base of the bladder
- makes part of seminal fluid
- creates a slightly basic (pH 7.5) fluid, high in fructose
5) Prostate Gland
- found around urethra
-prostaglandins (a hormone that causes contractions of the vagina to help move sperm), and buffers
6) Cowper's glands
- adds to seminal fluid
- 2 small glands
- secretes alkaline fluid to neutralise urine in urethra
* seminal fluid + sperm = semen
Seminal Fluid
- basic
- contains fructose (sugar) to prove energy for sperm swimming
- prostaglandins - hormone which causes mild contractions in uterus to help sperm move towards egg
7) Urethra
- double purpose tube (semen and urine), but never at same time
Semen is expelled out of urethra by rhythmic muscular contractions -> male orgasm
8) Penis
- becomes erect and hard to allow semen to be deposited in the vagina near the cervix
P2. PATH OF SPERM
1) Testes
2) Epididymis
3) Ductus (vas) deferens
5) Prostate Gland
7) Urethra
P3. FUNCTIONS OF SEMINAL FLUID
- lubricate the vagina
- provide energy for swimming sperm (fructose)
- stimulate mild contractions of the vagina (prostaglandins)
- buffers to counteract acidity in vagina and uterus
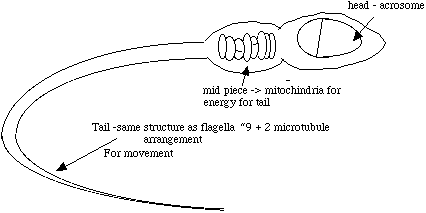
P4. SPERM
Acrosome or head contain 23 chromosomes and enzymes necessary for penetration of female egg surface
- outside abdominal cavity in scrotum
- sperm production needs < body temp
- sperm is produced inside tubes called seminiferous tubules
- interstilial cells also in testes produce male sex hormones -testosterone, and androgens
- maturing sperm are moved to the epididymis
2) Epididymis
- area where sperm mature (coiled tubes)
- then moved to the ductus (vas) deferens
3) Ductus (vas) deferens
- sperm stored here
- leads to urethra
- long tube from epid. to urethra
4) Seminal vesicles
- 2 small glands
- joins vas deferens at the base of the bladder
- makes part of seminal fluid
- creates a slightly basic (pH 7.5) fluid, high in fructose
5) Prostate Gland
- found around urethra
-prostaglandins (a hormone that causes contractions of the vagina to help move sperm), and buffers
6) Cowper's glands
- adds to seminal fluid
- 2 small glands
- secretes alkaline fluid to neutralise urine in urethra
* seminal fluid + sperm = semen
Seminal Fluid
- basic
- contains fructose (sugar) to prove energy for sperm swimming
- prostaglandins - hormone which causes mild contractions in uterus to help sperm move towards egg
7) Urethra
- double purpose tube (semen and urine), but never at same time
Semen is expelled out of urethra by rhythmic muscular contractions -> male orgasm
8) Penis
- becomes erect and hard to allow semen to be deposited in the vagina near the cervix
P2. PATH OF SPERM
1) Testes
2) Epididymis
3) Ductus (vas) deferens
5) Prostate Gland
7) Urethra
P3. FUNCTIONS OF SEMINAL FLUID
- lubricate the vagina
- provide energy for swimming sperm (fructose)
- stimulate mild contractions of the vagina (prostaglandins)
- buffers to counteract acidity in vagina and uterus
P4. SPERM
Acrosome or head contain 23 chromosomes and enzymes necessary for penetration of female egg surface
P5. FUNCTIONS OF TESTOSTERONE
- testosterone
- is the major hormone of the male
- develop and functioning of sex organs
- maturation of sperm
- second hair (facial hair, pubic etc.)
- voice deepens
- including muscle mass
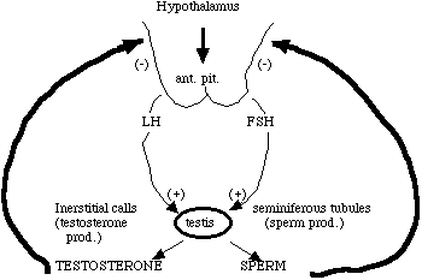
P6. CONTROL OF TESTOSTERONE
- control of testosterone levels is done by hypothalamus and gonadotrophic hormones from the ant. pituitary gland
- testosterone
- is the major hormone of the male
- develop and functioning of sex organs
- maturation of sperm
- second hair (facial hair, pubic etc.)
- voice deepens
- including muscle mass
P6. CONTROL OF TESTOSTERONE
- control of testosterone levels is done by hypothalamus and gonadotrophic hormones from the ant. pituitary gland
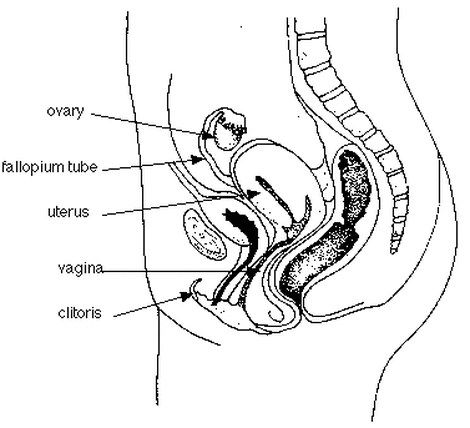
P7. STRUCTURE AND FUNCTION OF THE FEMALE
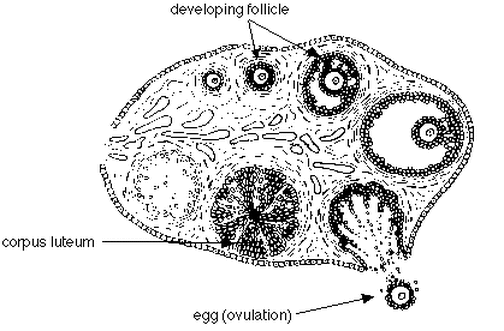
(1) The Ovaries - 2 Functions
(a) Produce eggs from follicles
(b) Produces sex hormones: estrogen (from follicles) & progesterone (from corpus lutem).
(1) The Ovaries - 2 Functions
(a) Produce eggs from follicles
(b) Produces sex hormones: estrogen (from follicles) & progesterone (from corpus lutem).
Note that this fig represents the sequences in 1 complete cycle (28 days) and that all these parts are not present at any one time.
(2) The fallopian tubes (Oviducts)
- connected to uterus & lie close to ovaries
- lined with cilia & surrounded by circular muscles
- purpose - (1) to propel egg toward uterus
(2) to serve as site of fertilization.
(3) Uterus (womb) - thick-walled, muscle lining - pear-shaped
- lined with a layer called the endometrium
- site of development of embryo.
(4) Cervix
- entrance to uterus
- path for sperm to swim through
- produces mucin strands to facilitate sperm
- also holds baby in the uterus
(5) Vagina
- birth canal
- recepticle for male's penis
(6) Clitoris
- sensitive organ analagous to male's penis
- respnsible for stimulating female orgasm
(2) The fallopian tubes (Oviducts)
- connected to uterus & lie close to ovaries
- lined with cilia & surrounded by circular muscles
- purpose - (1) to propel egg toward uterus
(2) to serve as site of fertilization.
(3) Uterus (womb) - thick-walled, muscle lining - pear-shaped
- lined with a layer called the endometrium
- site of development of embryo.
(4) Cervix
- entrance to uterus
- path for sperm to swim through
- produces mucin strands to facilitate sperm
- also holds baby in the uterus
(5) Vagina
- birth canal
- recepticle for male's penis
(6) Clitoris
- sensitive organ analagous to male's penis
- respnsible for stimulating female orgasm
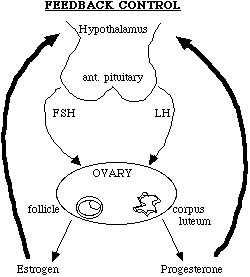
P8. The Female Hormones
1. Anterior Pituitary - makes 2 hormones that act on the ovaries
a) FSH - Follicle Stimulating Hormone - stimulates the follicle to mature and causes it to produce estrogen
b) LH - Leutinizing Hormone - maintains the corpus luteum and causes it to produce estrogen
- these are the Gondadotrophic Hormones (FSH & LH)
- they regulate the ovary's production of female sex hormones
2. Ovary - makes 2 hormones that act on the endometrium (uterus lining)
a) Estrogen (made by the follicle)
b) Progesterone (made by the corpus luteum)
Functions of Estrogen
stimulates:
- growth of uterus and vagina
- secondary sex characteristics (body hair, fat distribution, increased pelvic girdle, breasts)
- egg maturation
- endometrium thickening
1. Anterior Pituitary - makes 2 hormones that act on the ovaries
a) FSH - Follicle Stimulating Hormone - stimulates the follicle to mature and causes it to produce estrogen
b) LH - Leutinizing Hormone - maintains the corpus luteum and causes it to produce estrogen
- these are the Gondadotrophic Hormones (FSH & LH)
- they regulate the ovary's production of female sex hormones
2. Ovary - makes 2 hormones that act on the endometrium (uterus lining)
a) Estrogen (made by the follicle)
b) Progesterone (made by the corpus luteum)
Functions of Estrogen
stimulates:
- growth of uterus and vagina
- secondary sex characteristics (body hair, fat distribution, increased pelvic girdle, breasts)
- egg maturation
- endometrium thickening
These feedback controls are more complicated than the male and do nor try to maintain homeostasis. Hormone levels may vary.
P9. & P10. The Female cycles
- there are two cycles -> i) Ovarian cycle
ii) Menstrual cycle
i) Ovarian cycle (28 days average)
Days 1-14
-FSH released from ant. pit.
- stimulates the development of a follicle (unfertilized egg)
- follicle begins to secrete estrogen , so the level of this hormone steadily increased
Day 14
- follicle releases egg -> Ovulation (a peak of LH from ant. pit. stimulates this)
Day 15-28
- follicle turns into corpus luteum
- LH from ant. pit. stimulates the production of progesterone
- as progesterone increases, ant. pit. decreased LH so corpus luteum begins to degenerate
- when corpus luteum is gone, menstration occurs
ii) Menstrual Cycle
Days 1-5
- low level of estrogen and progesterone
- cause thickened uterine lining to degenerate and shed menstration "period'
Days 6-13
- estrogen (from follicle) is increasing which causes a thickening of the uterus wall (endometrium)
- extra blood vessels and glands
Day 14
- Ovulation
Day 15-28
- increased levels of progesterone causes endometrium to thicken further (2x) and thick mucoid secretion
- endometrium is ready to receive fertilized egg (zygote)
NORMALLY ->
- egg is not fertilized therefore copus luteum begins to degenerate therefore progesterone falls
- low progesterone and estrogen cause endometrium to be shed. Menstration begins
P12. Implantation
- fertilized egg attaches to endometrium (uterus lining) several days after fertilization
- hormones are produced by the zygote to prevent menstruation
- HCG - Human Chorionic Gonadotrophin is the hormone, and it maintains the corpus luteum which continues to produce estrogen which prevents the endometrium from shedding. Pregnancy test uses monoclonal antibodies to test for this hormone.
- corpus luteum persists for 3 - 6 months
- endometrium and fetus develop the plaecenta (organ of exchange between maternal and fetal blood systems)
- the placenta continues production of HCG, and also produces prog . and estrogen . Higher levels of these 2 hormones shut of release of FSH from ant. pit. preventing ovulation and maintaining the endometrium. (Birth control pill does this too)
P11. Oxytocin
Oxytocin is a hormone produced by the Posterior pituitary gland . It is controlled by a positive feedback system. In a positive feedback system, the level of the hormone in the blood feeds back to the post. pit. and increases release of Oxytocin. Oxytocin is responsible for causing the uterus to contract during birth. Thus, one birth contraction stimulates the release of more oxytocin, which leads to a stronger, closer contraction, which stimulates the release of more oxytocin and so on. Thus, birth contractions get stronger and closer until the birth of the baby. A positive feedback system is unstable and does not lead to homeostasis. They are rare in the human body.
P9. & P10. The Female cycles
- there are two cycles -> i) Ovarian cycle
ii) Menstrual cycle
i) Ovarian cycle (28 days average)
Days 1-14
-FSH released from ant. pit.
- stimulates the development of a follicle (unfertilized egg)
- follicle begins to secrete estrogen , so the level of this hormone steadily increased
Day 14
- follicle releases egg -> Ovulation (a peak of LH from ant. pit. stimulates this)
Day 15-28
- follicle turns into corpus luteum
- LH from ant. pit. stimulates the production of progesterone
- as progesterone increases, ant. pit. decreased LH so corpus luteum begins to degenerate
- when corpus luteum is gone, menstration occurs
ii) Menstrual Cycle
Days 1-5
- low level of estrogen and progesterone
- cause thickened uterine lining to degenerate and shed menstration "period'
Days 6-13
- estrogen (from follicle) is increasing which causes a thickening of the uterus wall (endometrium)
- extra blood vessels and glands
Day 14
- Ovulation
Day 15-28
- increased levels of progesterone causes endometrium to thicken further (2x) and thick mucoid secretion
- endometrium is ready to receive fertilized egg (zygote)
NORMALLY ->
- egg is not fertilized therefore copus luteum begins to degenerate therefore progesterone falls
- low progesterone and estrogen cause endometrium to be shed. Menstration begins
P12. Implantation
- fertilized egg attaches to endometrium (uterus lining) several days after fertilization
- hormones are produced by the zygote to prevent menstruation
- HCG - Human Chorionic Gonadotrophin is the hormone, and it maintains the corpus luteum which continues to produce estrogen which prevents the endometrium from shedding. Pregnancy test uses monoclonal antibodies to test for this hormone.
- corpus luteum persists for 3 - 6 months
- endometrium and fetus develop the plaecenta (organ of exchange between maternal and fetal blood systems)
- the placenta continues production of HCG, and also produces prog . and estrogen . Higher levels of these 2 hormones shut of release of FSH from ant. pit. preventing ovulation and maintaining the endometrium. (Birth control pill does this too)
P11. Oxytocin
Oxytocin is a hormone produced by the Posterior pituitary gland . It is controlled by a positive feedback system. In a positive feedback system, the level of the hormone in the blood feeds back to the post. pit. and increases release of Oxytocin. Oxytocin is responsible for causing the uterus to contract during birth. Thus, one birth contraction stimulates the release of more oxytocin, which leads to a stronger, closer contraction, which stimulates the release of more oxytocin and so on. Thus, birth contractions get stronger and closer until the birth of the baby. A positive feedback system is unstable and does not lead to homeostasis. They are rare in the human body.